Your Nuclear Oncologist
In a recent email message, Wong congratulated Division and DCI colleagues for their “tireless work” on achieving the Comprehensive Radiopharmaceutical Therapy Center of Excellence designation and for “making Duke a leader in this field.”
He stresses that the Division of Nuclear Medicine and Radiotheranostics is only one component of the Comprehensive Radiopharmaceutical Center of Excellence recognition.
“It is important to note that our Division is fully integrated with the Duke Cancer Institute, working closely with the neuroendocrine GI Oncology group and the DCI Center for Prostate & Urologic Cancers,” says Wong. “Patients at DCI are evaluated by multidisciplinary teams to provide individualized treatment plans and to determine whether radiopharmaceutical therapy is the best option.”
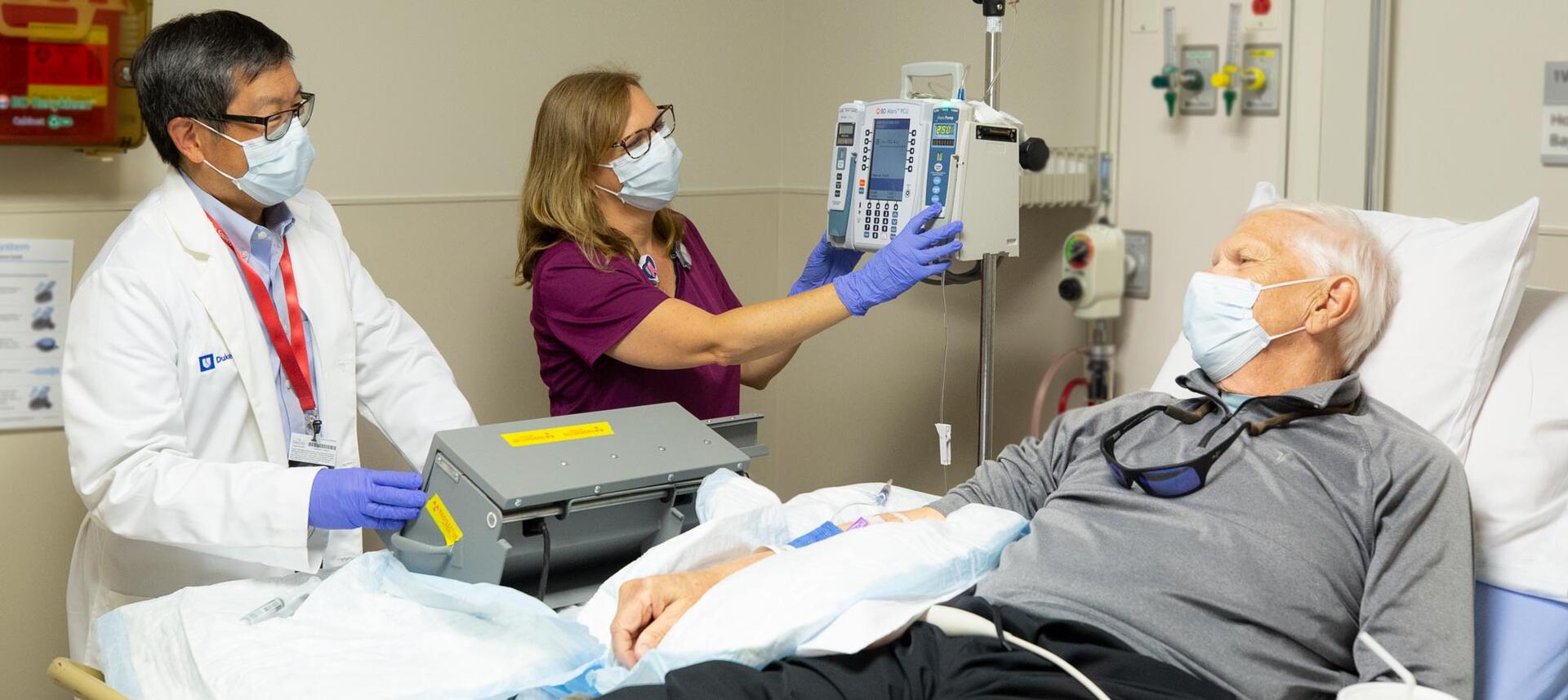
In addition to an experienced team of nuclear medicine physicians, technologists, nurses, and physician assistants, Duke has a dedicated Radiopharmacy to manage ordering and scheduling the delivery of radiotracers and radiopharmaceuticals. Every high dose radiopharmaceutical administration is also overseen by a member of the Duke Radiation Safety Division who meets with the patient to provide individualized post-treatment recommendations.
The SNMMI website lists the Comprehensive Radiopharmaceutical Therapy Centers of Excellence, provides educational resources (research articles and continuing education) about radiopharmaceutical therapies for technologists and has recently added a Patient Resources portal where patients and families can access easy-to-understand fact sheets, guidelines, and informational videos to help better understand nuclear medicine treatment.
“The goal of the (SNMMI) program is to ensure patients have reliable access to high quality radiopharmaceutical therapy, well-integrated into their pathway of care, delivered by highly qualified therapy teams, at technically qualified sites, and led by physicians appropriately trained in nuclear medicine acting as the patient’s ‘nuclear oncologist,’” wrote SNMMI president Richard L. Wahl, MD, FACR, in an official letter this May notifying Wong of the newly-earned designation. “SNMMI is delighted that you and your colleagues share in this important endeavor.”