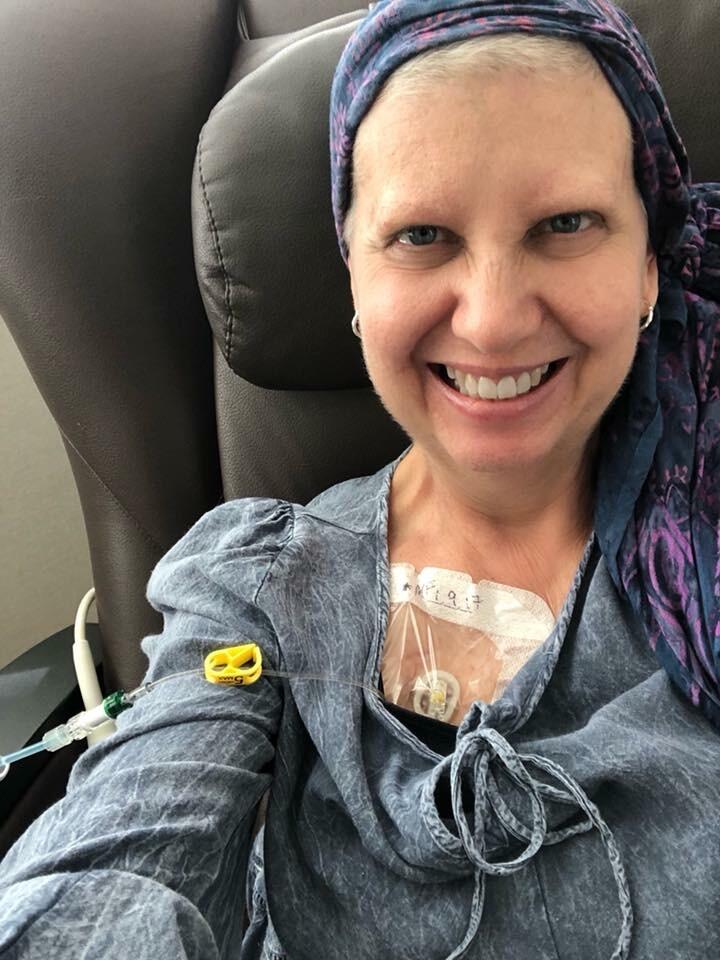
Diagnosed with stage 4 ovarian cancer three years ago, Kathy Jennings was thrown a lifeline when she came to Duke Cancer Center.
It’s October 30, 2019. The pre-pandemic “before times” in the expansive fourth-floor waiting room of the Oncology Treatment Center, Duke Cancer Center, Durham.
Volunteers in Duke blue vests are handing out coffee and making small talk with patients waiting to be called for their next IV infusion of cancer-fighting drugs — treatments they hope will ultimately prolong their life, if not cure them.
Kathy Jennings, 59, is there to support a friend at her first chemotherapy appointment.
It’s been almost two years to the day since Jennings’ final chemotherapy treatment for ovarian cancer.
“It was rough having chemo every week and I forget how harsh the side effects are until I begin helping a friend with their journey,” says the vibrant cancer survivor, agreeing to be interviewed about her own journey before she joins her friend in the treatment room.